Patient Experience in the Dental Practice: 4 Details That Drive Case Acceptance
There is a contradiction in every dental practice: you can be the best clinician in your city, but your patient lacks the tools to understand it.
They don’t have the eye to evaluate the precision of your margin integrity, they can’t read a periapical X-ray, and they don’t perceive the difference between a successful impression and a mediocre one.
The patient experience in your dental practice is based exclusively on something far more refined than one might think: a nervous system that records every tactile, visual, and olfactory sensation, and a mind that transforms those sensations into instant judgments about your professional value.
The SERVQUAL model, one of the most robust frameworks for analyzing perceived quality in healthcare, proves this with data in hand: patients build trust in a professional through indirect signals (the so-called trust proxies) far more than through the evaluation of direct clinical competence.

In other words, the patient does not buy your treatment. They buy the feeling of being in good hands.
With this deep dive, we want to help you see your practice through the eyes of the patient: a point of observation that is sometimes uncomfortable, often surprising, and always useful.
We will analyze 4 psychological breaking points where, unconsciously, you lose the patient’s trust before they have even read the quote.
Optimizing the patient experience in the dental practice is not an aesthetic whim. It is the lever with the best cost/benefit ratio to increase case acceptance.
The first physical contact: why the impression tray tells the whole story
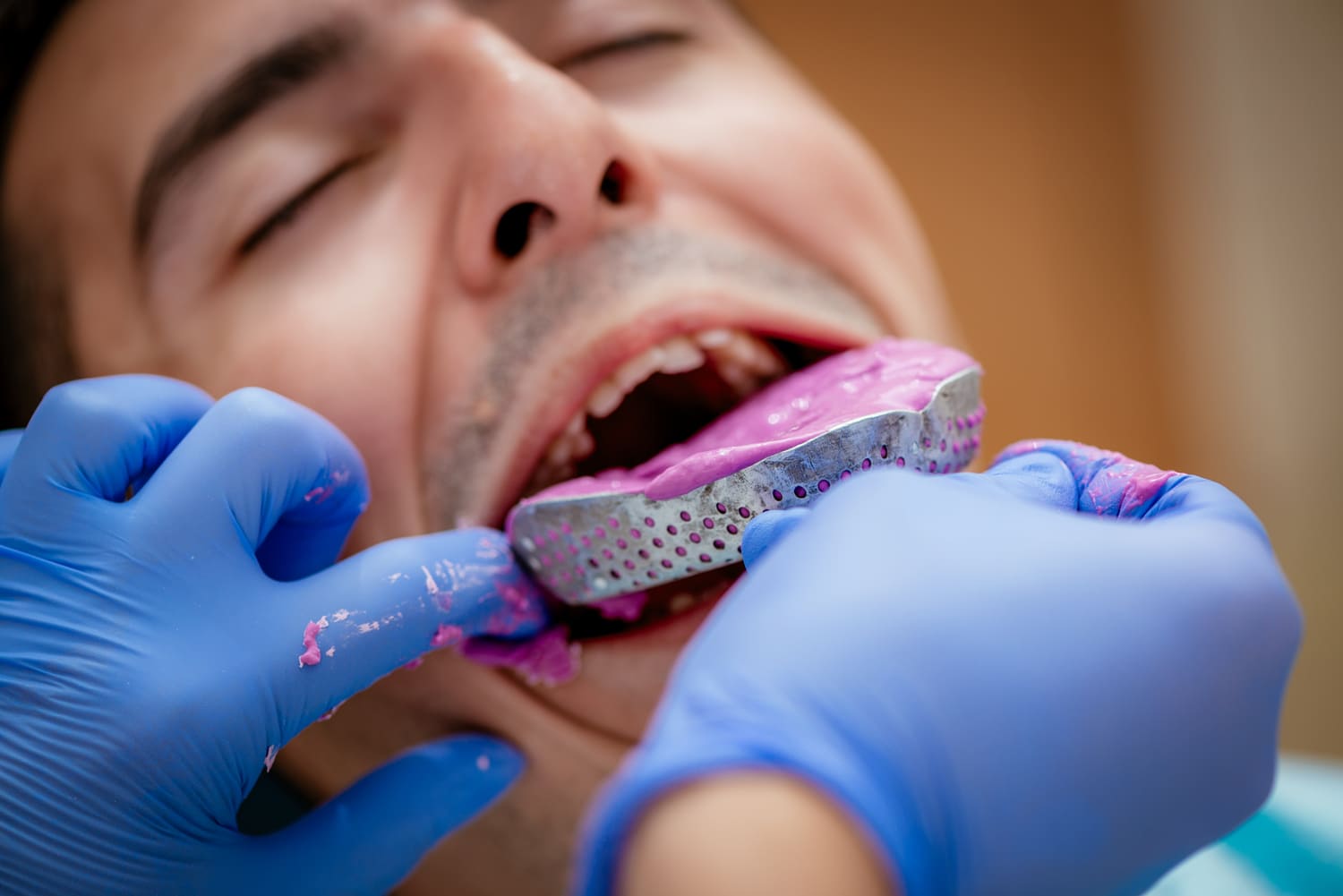
Think about the last time you took an impression. For you, it’s a routine clinical act, probably performed a million times, but for the patient in front of you—who might be having their first impression ever—it’s a new and, most likely, not exactly pleasant sensory experience.
The coldness of the metal, the metallic taste of traditional trays, the tactile sensation of a rigid and “hospital-like” object, the alginate or silicone that feels like it’s sliding down the throat: all of this activates the patient’s nervous system in alert mode. And a patient on alert is a patient who struggles more to lower their defenses, listen to the treatment proposal, and sign the quote without resistance.
Consumer psychology calls this mechanism “sensory priming”: the first physical sensations of an experience emotionally color everything that follows.
If the first physical contact with your practice is cold—literally—the patient will use that sensation as a yardstick for the rest of the visit.
How is this solved in practice?

The use of disposable impression trays made of non-toxic material, besides being a matter of hygiene (and the hygiene of disposables, in terms of patient experience, is already a powerful message: “this tool is only for me”), is also a matter of thermal comfort and perceived temperature.
A tray that doesn’t taste like metal and doesn’t transmit instant cold lowers the patient’s anxiety threshold before you’ve even said a word.
Concrete result: a patient who is less “on guard” is more receptive to clinical communication, asks fewer defensive questions, and tends to accept the treatment plan with less resistance.
Your impression tray, used well, becomes one of your best collaborators in managing the patient experience in dentistry.
The wide-open mouth: the ergonomics the patient will never tell you about

Let’s face it: holding the mouth open by force for twenty, thirty, or forty minutes is a form of prolonged muscle tension that the body does not easily forget.
The brain associates that physical fatigue with a stressful experience, and the dental practice enters the patient’s memory as a place of suffering, even when clinically everything went perfectly. Yet, this is one of the most underestimated components of the patient experience in the dental practice.
The reason is simple: the patient rarely says it. They don’t protest, they don’t complain, because they are there to be treated and they know that a certain degree of discomfort is part of the game. But they remember it. And when it’s time to sign the quote for the next treatment, that physical memory carries weight—even unconsciously.
The change of perspective that changes everything

Mouth props and lip retractors are often considered ergonomic tools for the clinician: they improve visibility of the operative field, facilitate work, and reduce operator fatigue.
All true. But there is a second level of reading worth exploring.
For the patient, having a support that “holds” the mouth open for them means delegating muscle tension to an external tool.
They no longer have to exert active effort. The muscles relax. And when the muscles relax, even the perception of time changes: a thirty-minute procedure with a mouth prop is often remembered as “fast and painless,” even when objectively it was neither very short nor completely devoid of sensation.
This is dental marketing in its most authentic form: a physical experience that generates a positive judgment.
The patient won’t say “thank you for the mouth prop.” But they will return with more peace of mind.
3. The tongue’s microscope: how the patient evaluates your clinical excellence

This is the point where many professionals are surprised. The patient has no real way to quantify the precision of your restoration. They don’t have a magnifying lens to evaluate margins, nor a caliper for precision and alignment.
However, they have an extraordinary, evolutionarily refined instrument that they use consistently, systematically, before even leaving the chair: The tip of the tongue. Capable of detecting surface differences on a micron scale. Far more sensitive than the touch of a hand. A restoration that is not perfectly polished, even if clinically flawless, is perceived by the tongue as “rough,” “coarse,” or “strange. And the patient translates that tactile perception into an immediate qualitative judgment: “the work is not perfect.” Because perceived quality—the core concept of any customer experience analysis—is built on available sensory signals, not on objective technical competence.
The tactile signature of excellence
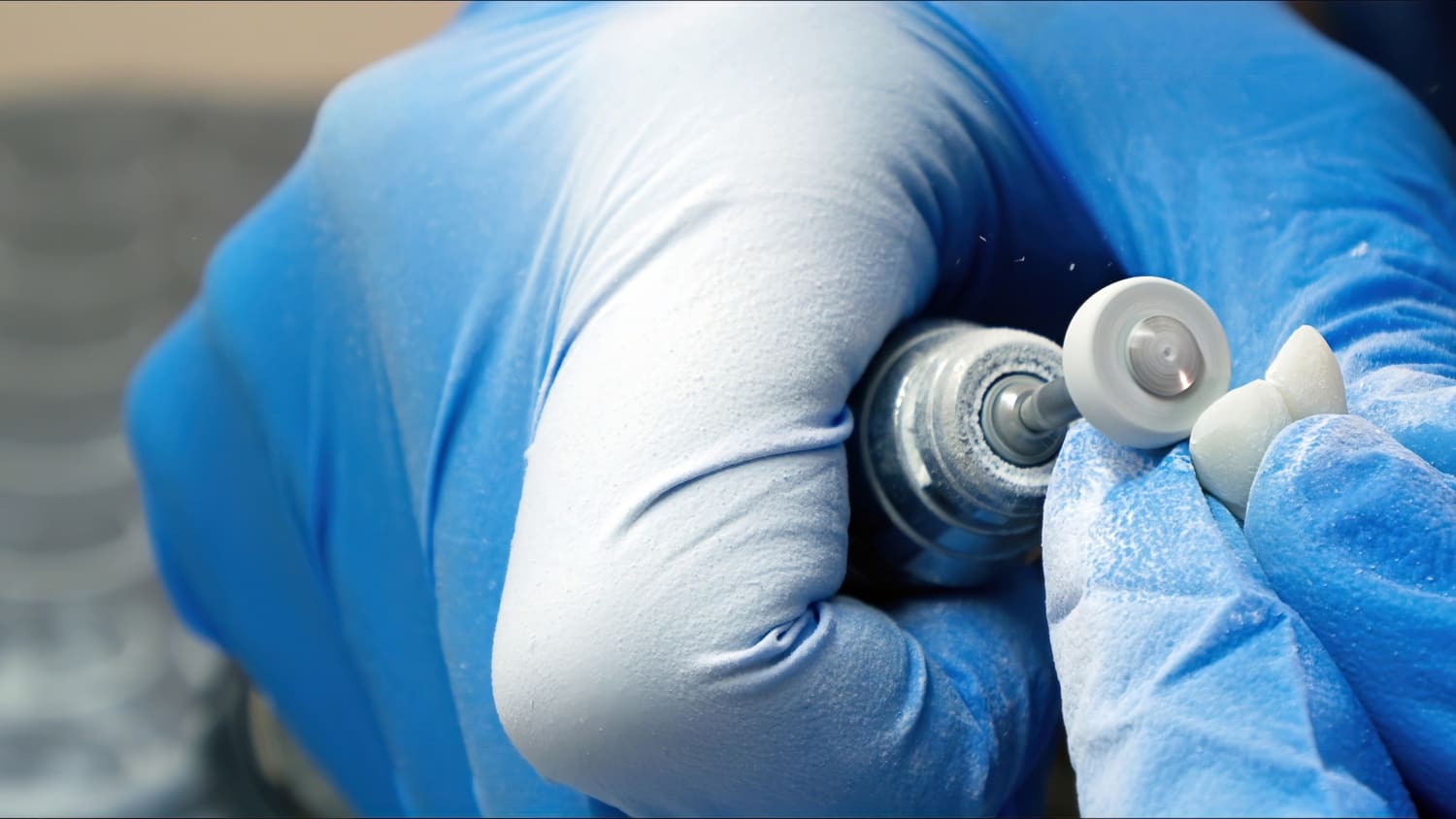
The mirror-like polishing of a restoration is not an aesthetic whim reserved for perfectionists. It is the tactile signature of your clinical quality.
Every time the patient passes their tongue over the restoration and feels no difference compared to the natural tooth, they are receiving a sensory confirmation of your excellence—even if they will never know they received it. Professional tools such as convergent bristle brushes and specific polishing brushes allow you to reach that level of surface quality that the patient’s tongue perceives as natural. It is an investment of a few minutes of clinical time, with a direct return on the perceived quality of the dental practice and on the patient’s propensity to accept the subsequent treatment plan.
4. Clinical language: when words become a wall

“Pass me the 15 blade, then the coarse diamond bur, then the bonding agent.” Perfectly normal for you.
For the patient lying in the chair, eyes fixed on the ceiling, it is a stream of unknown words that the brain processes in only one direction: “what is he about to do to me with that thing?” An unidentified danger.
Verbal exclusion, the clinical chatter over the patient’s head, is one of the most underestimated mechanisms in the analysis of the patient experience in dentistry. A patient who doesn’t understand what is being said around them doesn’t feel at the center of the care: they feel like a “case” to be managed.
And a patient who feels like a case, not a person, has less empathy for the professional and less trust in the quote they will be offered.
Communicating without excluding: the visual protocol

The solution is not to eliminate technical language from the clinical dialogue (which is logistically impossible and clinically counterproductive), but rather to build shared visual protocols between the dentist and the Dental Assistant (DA) that minimize the need to verbalize every step over the patient’s head.
Trays organized in operative sequence, instruments arranged with a recognizable visual logic, non-verbal signals agreed upon with the team: these are micro-organizational changes in the dental practice organization that have a direct effect on patient perception.
Less chatter means less anxiety, more sense of control, and a greater propensity to listen to the clinical proposal.
Effective dentist-patient communication begins with how you organize the silence around them.
Humble details are your best salespeople
Increasing the quote acceptance rate doesn’t necessarily require new presentation software, 4K screens to show X-rays, or color brochures.
It requires something harder to buy: the ability to see your practice through the patient’s senses.
An impression tray that doesn’t taste like metal. Muscles that are not tortured by forty minutes of tension. A restoration that the tongue perceives as natural. An environment where the patient understands what is happening around them.
These cannot just be details. In fact, they are the trust proxies the patient uses to build their judgment of you.
That judgment, formed before you have even opened your mouth to present the treatment plan, already decides 70% of the response to your quote.
The patient buys the treatment but also the feeling of being in good hands. Every well-managed sensory detail is a silent argument in favor of your quote.
Start with one of these four points.
Implement the change systematically and measure the difference in patient feedback in the following weeks. The results, usually, arrive sooner than expected.
Here are a few products to help you refine those small, yet essential, details that patients notice most
-
Cheek retractors
0,00 € -
MT
0,00 € -
Cheek retractors with long handles
0,00 €
FAQ – Frequently Asked Questions
Yes, significantly. Research in health marketing (including those based on the SERVQUAL model) shows that patient trust—and therefore their propensity to accept a treatment plan—depends largely on indirect perceptual signals: physical comfort, perceived hygiene, and communicative clarity. Objective clinical competence is evaluated only secondarily because the patient lacks the tools to do so directly.
They are indirect indicators through which the patient evaluates the quality of the professional. Unable to judge the precision of a restoration or the correctness of a diagnosis, the patient uses accessible signals: the tactile sensation of the instruments, the order of the tray, the comfort of the chair, and the team’s tone of voice. Optimizing these signals is a concrete form of dental marketing applied to the patient experience.
By working on perceived quality before the presentation of the quote. Patients who experience a comfortable, orderly, and anxiety-free visit are statistically more predisposed to accept the proposed treatment plan because they have already built implicit trust in the professional. Details like accurate polishing of restorations, the use of comfortable instruments, and clear communication with the Dental Assistant directly impact this perception.
Besides empathetic verbal communication, acting on the sensory signals of the clinical environment is among the most effective strategies. Reducing background noise during procedures, using instruments with a reassuring tactile profile, delegating muscle tension to supports like mouth props, and organizing the operative field in an orderly manner all contribute to reducing the activation of the patient’s autonomic nervous system—which is the main cause of dental anxiety.
More than one might think. The human tongue is capable of detecting surface differences on a micron scale—far more than the fingertips. A restoration that is not perfectly finished is perceived by the patient as ‘rough’ or ‘incomplete,’ even if it is clinically excellent. Mirror-like polishing is the tactile signature of clinical quality: the patient perceives it even without being able to name it, and uses it as a proxy to evaluate the excellence of the practice.



